Venous thromboembolism is a major problem after surgery, but we may have ignored a major factor: Red blood cell transfusion! Dr. Ruchika Goel discusses her very important article in JAMA Surgery.
NOTE: Continuing Education credit for this episode has expired. See below for details.

Dr. Ruchika Goel
Do RBC Transfusions Impact VTEs?
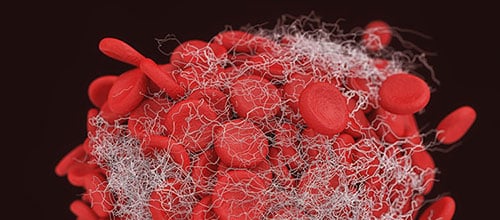
Recent publications (including the “TRANSFUSION-2” study) have illuminated the possibility that red blood cell transfusion might play a bigger role in the development of VTEs than previously thought. RBCs may not just be “innocent bystanders” caught in a web of blood clot formation; they could actually contribute to inflammation and hypercoagulation. Ruchika and Aaron Tobian joined with an “all-star” group of Transfusion Medicine experts for the first study to primarily address the role of perioperative red blood cell transfusions in developing postoperative venous thromboemboli. Ruchika is here to tell us what they found.

Dr. Ruchika Goel
Do RBC Transfusions Impact VTEs?
Recent publications (including the “TRANSFUSION-2” study) have illuminated the possibility that red blood cell transfusion might play a bigger role in the development of VTEs than previously thought. RBCs may not just be “innocent bystanders” caught in a web of blood clot formation; they could actually contribute to inflammation and hypercoagulation. Ruchika and Aaron Tobian joined with an “all-star” group of Transfusion Medicine experts for the first study to primarily address the role of perioperative red blood cell transfusions in developing postoperative venous thromboemboli. Ruchika is here to tell us what they found.
About My Guest:
Ruchika Goel MD MPH is board-certified in Pediatrics, Pediatric Hematology/Oncology, and Blood Banking/Transfusion Medicine. Her training included a pediatrics residency at Children’s Hospital of Pittsburgh, pediatric Hematology/Oncology fellowship at Johns Hopkins, and Blood Banking/Transfusion Medicine fellowship at New York Presbyterian Hospital, Weill Cornell Medical College, and the New York Blood Center.
Ruchika is a member of the Hematology-Oncology faculty at the Simmons Cancer Institute at Southern Illinois University. She is also Associate Medical Director of the Mississippi Valley Regional Blood Center, and Adjunct Assistant Professor of Pathology in the Division of Transfusion Medicine at Johns Hopkins University. Ruchika has received multiple awards for her medical research, and has numerous publications in peer-reviewed journals and books in both Transfusion Medicine and Pediatrics. She serves on the AABB Clinical Transfusion Medicine Committee (contributing to the article discussed in episode 055CE of this podcast), the AABB Pediatric Subsection Committee, and the ISBT Clinical Transfusion Pediatric Group Working Party.
Continuing Education Expired
This podcast episode offered continuing education credit for two years from its release date, but is no longer eligible for such credit.
To find Blood Bank Guy Essentials Podcast episodes with active continuing education opportunities, Click here or visit Transfusion News Continuing Education on Wiley Health Learning.
DISCLAIMER: The opinions expressed on this episode are those of my guest and I alone. They do not necessarily reflect those of the organizations with which either of us is affiliated. Neither Dr. Goel nor I have any relevant financial disclosures.
The images below are generously provided by Dr. Goel.
Further Reading:
- Article discussed in this interview: Goel R, Patel EU, Cushing MM, et al. Association of Perioperative Red Blood Cell Transfusions With Venous Thromboembolism in a North American Registry. JAMA Surgery 2018;153(9):826–833.
- Research letter in JAMA outlining US blood use trends: Goel R, et al. Trends in Red Blood Cell, Plasma, and Platelet Transfusions in the United States, 1993-2014. JAMA 2018;319(8):825-827.
- 2014 study showing RBC transfusion may increase in-vitro platelet activation and aggregation: Silvain J et al. Impact of Red Blood Cell Transfusion on Platelet Aggregation and Inflammatory Response in Anemic Coronary and Noncoronary Patients. J Am Coll Cardiology 2014;63(13):1289-1296.
Music Credit
Music for this episode includes “Cuando te invade el temor” and “Reflejo,” both by Mar Virtual via the Free Music Archive. Click the image below for permissions and license details.

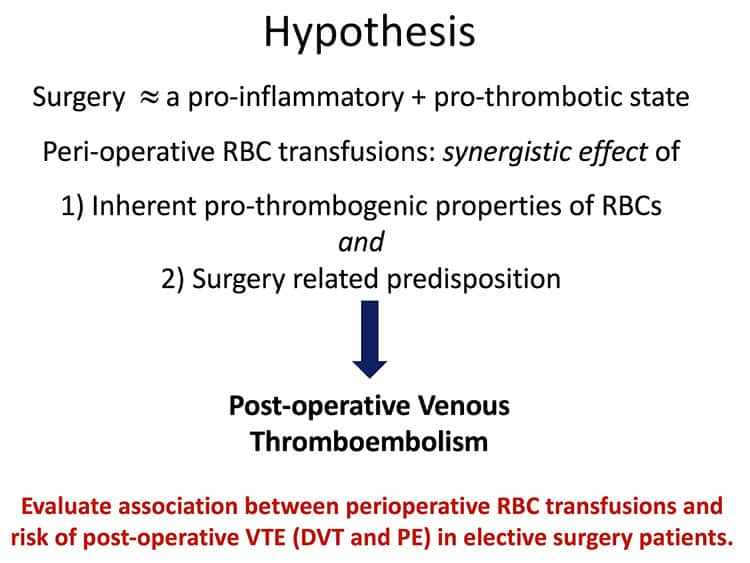
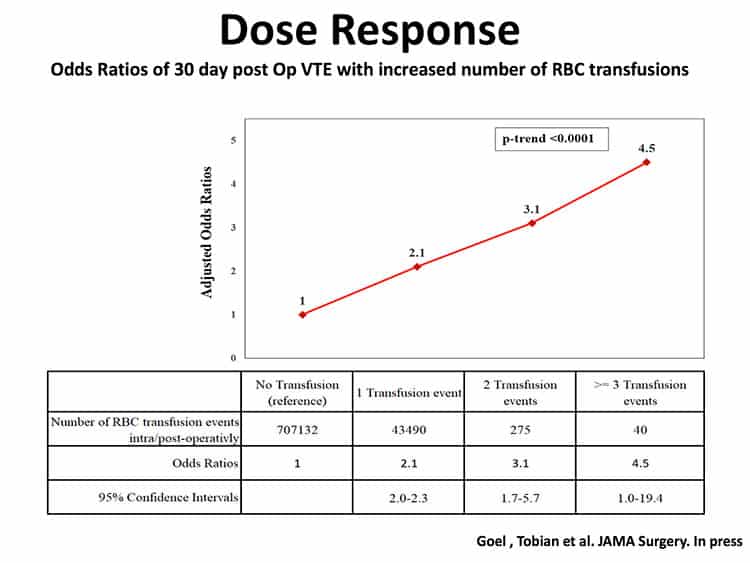

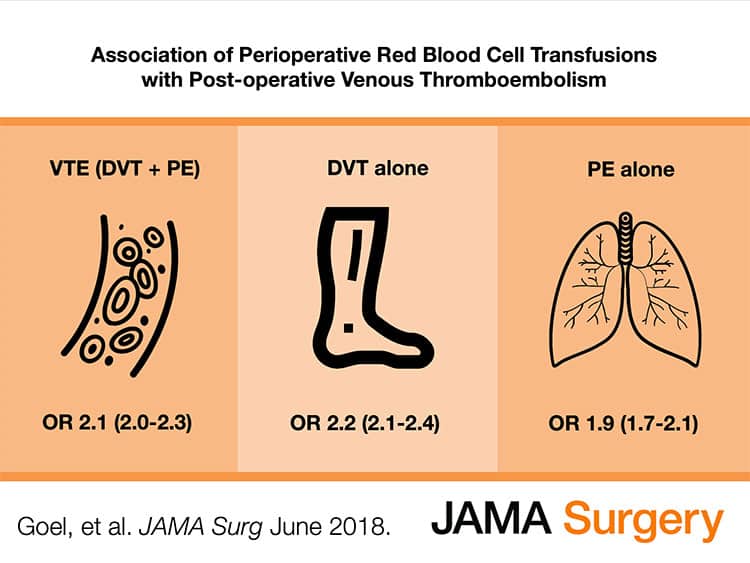



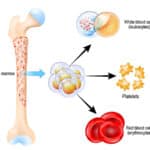





Nice addition to the literature on this subject, and another reason not to lightly transfuse patients for fatigue or similar non-life threatening symptoms, except perhaps at the end of life..
Thrombosis has been convincingly shown to be associated with red cell transfusion in a randomized trial, as well as in some previous cohort studies. The same is true to some extent of cohort studies of platelet transfusion and plasma transfusion. Transfusions are pro-inflammatory and inflammation and thrombosis are closely linked both mechanistically and clinically.
JAMA. 2014 Jul 2;312(1):36-47. doi: 10.1001/jama.2014.6490.
Effect of erythropoietin and transfusion threshold on neurological recovery after traumatic brain injury: a randomized clinical trial.
“There was a higher incidence of thromboembolic events for the transfusion threshold of 10 g/dL (22/101 [21.8%] vs 8/99 [8.1%] for the threshold of 7 g/dL, odds ratio, 0.32 [95% CI, 0.12 to 0.79], P = .009).”
Association between delivery methods for red blood cell transfusion and the risk of venous thromboembolism: a longitudinal study.
Lancet Haematol. 2016 Dec;3(12):e563-e571. doi: 10.1016/S2352-3026(16)30132-6.
As always, thanks for your thoughts, Neil!
-Joe
Dear Dr. Blumberg,
Thank you for your excellent and insightful comment.
Thank you, again Joe!
Warm regards,
Ruchika
enjoyed