Trauma transfusions require prompt delivery of plasma. To conserve resources, many transfusion services have started using group A plasma instead of AB in these emergency settings. But, is the practice safe?

Dr. Nancy Dunbar and Dr. Tait Stevens
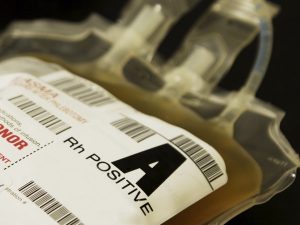
Over the last ten years or so, the world of trauma transfusion has undergone nothing short of a revolution. We’ve heard all about the famous “1:1:1” ratio of platelets to plasma to red cells that has become standard practice in massive trauma transfusion (described in BBGuy Essentials episodes 007 and 033). One of the dirty little secrets of this whole situation is that we are using more plasma than before (shown in published studies). With more overall demand comes more demand for group AB plasma, in addition, since AB has traditionally been considered the “universal” plasma component to give when you don’t know someone’s ABO type. However, since AB donors only make up about 4% of our donor pool, keeping up can be a struggle!
Group A to the Rescue?
About My Guests:
Dr. Nancy Dunbar is an associate professor of pathology and lab medicine and a clinical assistant professor of medicine at Dartmouth. She is lead author, along with Mark Yazer, of a paper called, “Safety of the use of group A plasma in trauma: The STAT study” that is currently in early view publication for the journal Transfusion (08/07/2017 UPDATE: The paper is now published in the August 2017 Transfusion; see link below).
Dr. Tait Stevens is an associate professor of pathology and lab medicine at Loma Linda University. He is the director of Transfusion Medicine and the histocompatibility lab at Loma Linda. Tait is lead author of a paper called, “Incompatible type A Plasma Transfusion in Patients Requiring Massive Transfusion Protocol: Outcomes of an EAST Multicenter Study” published in July 2017 in the Journal of Trauma and Acute Care Surgery.
Take the Quiz and See What You Learned!
Further Reading:
- Dr. Dunbar’s Paper: Dunbar NM and Yazer MT, on behalf of the Biomedical Excellence for Safer Transfusion (BEST) Collaborative and the STAT Study Investigators. Safety of the use of group A plasma in trauma: the STAT study. Transfusion 2017;57;1879–1884.
- Dr. Stevens’ Paper: Stevens WT et al. Incompatible type A plasma transfusion in patients requiring massive transfusion protocol: Outcomes of an Eastern Association for the Surgery of Trauma multicenter study. J Trauma Acute Care Surg 2017;83(1):25-29.
- Survey of Current Practice Mentioned by Dr. Dunbar: Dunbar NM, Yazer MH. A possible new paradigm? A survey-based assessment of the use of thawed group A plasma for trauma resuscitation in the United States. Transfusion 2016; 56:125-9.
Previous Literature on this Issue (cited in blog post)
- Chhibber V et al. Is group A plasma suitable as the first option for emergency release transfusion? Transfusion 2014;54:1751-5.
- Cooling L. Going from A to B: The safety of incompatible group A plasma for emergency release in trauma and massive transfusion patients. Transfusion 2014;54:1695-1697.
- Isaak EJ, et al. Challenging dogma-Group A donors as universal plasma in massive transfusion protocols. Immunohematology 2011;27:61-65 (NOTE: Free pdf download of full issue).
- Mehr CR, Gupta R, von Recklinghausen FM, et al. Balancing risk and benefit: maintenance of a thawed group A plasma inventory for trauma patients requiring massive transfusion. J Trauma Acute Care Surg 2013;74:1425-31.
- Zielinski MD et al. Emergency use of prethawed group A plasma in trauma patients. J Trauma Acute Care Surg 2013;74:69-75.









Thank you for producing the podcast highlighting studies involving ABO incompatible plasma use in trauma and massive transfusion settings. Towards the end of the podcast there is discussion of a desire for better compatibility screening tools.
Your audience may be interested in publications demonstrating the usefulness of the CHUHE assay, including:
“Discriminating the hemolytic risk of blood type A plasmas
using the complement hemolysis using human erythrocytes
(CHUHE) assay” Volume 57, March 2017 TRANSFUSION
In addition to plasma screening, this assay has also helped explaining why some group O RBC units cause more hemolysis when given to non-O patients than others, independent of simple donor antibody titer.
Thanks for sharing, Mike! I admit that I just breezed over this article in the March 2017 Transfusion. Very interesting! Not quite the ultra-quick solution Dr. Stevens mentioned in the podcast, but a potential aid in the evaluation. I’m not aware of many centers doing at this point, but this is valuable information.
NOTE to everyone: I verified with Mike that he has no financial or research connections to this assay. He is, as he puts it, “a human blood banker with a strong bias against hemolysis, renal damage, and other transfusion associated harm, and towards providing the safest most efficacious treatment possible.”
-Joe
A better strategy for the patient in this paper would have been to give ABO identical (group B) red cells. There is no medical or logistic reason for giving ABO mismatched plasma for an elective transfusion, as seems to have been done in this case. Our blithe use of universal group O donor red cells when the ABO of the patient is known is based upon no evidence of safety whatever. Indeed we know that a finite number of individuals will have serious or even fatal reactions to this small amount of incompatible plasma. With all due respect, I would suggest we don’t primarily need better assays, we need better transfusion choices, contrary to a century of practice.
Dear Joe excellent. Thank you very much and alot of thanks to Dr. Nancy Dunbar and Dr. Tait Stevens.
Glad you enjoyed it. They are two brilliant physicians, and I was honored to learn from both of them.
-Joe
I think the evidence that A plasma is no worse than AB plasma in trauma patients of unknown ABO type is reasonably convincing, contrary to the editorial in TRANSFUSION on the subject, claiming this practice violates the precautionary principle.
I also suspect that what is not being fully appreciated is that while A plasma is no worse than AB plasma, it may still be substantially inferior to ABO identical plasma. Our rationale is really quite simple. Swedish investigators demonstrated that group O recipients of larger volumes of AB plasma (5 units or more) had a 9% increase in mortality rate in their national registry (Vox Sang. 2009 May;96(4):316-23). Inaba and colleagues have similar data showing an association between ABO compatible plasma and increased ARDS and sepsis (Arch Surg. 2010 Sep; 145(9):899-906. PMID: 20855762).
AB plasma has soluble antigen (at least in secretors) incompatible with 95% of recipients’ plasma isoagglutinins. ABO immune complexes have been shown to likely cause increased bleeding (in clinical studies), impair platelet function, clot formation, endothelial cell integrity, and cause hemolysis (in vitro)(reviewed in Blood Transfusion = Trasfusione del sangue.2015 Jul 0; 13(3):347-50).
A plasma is only incompatible with 60% of recipients in this way, compared with 95% for AB plasma, so it would not be surprising if they gave clinically equivalent (but not optimal) results.
Thank you very much for your comment, Dr. Blumberg. Your perspective is appreciated, as always, as are your points about the soluble antigen incompatibility with recipient plasma.
-Joe
I just found your Podcast and am delighted to have this resource.
I am affiliated with 2 community hospitals, one a level 1 trauma center, the second a level 2 trauma center. We have instituted providing group A plasma in our trauma massive transfusion coolers in the past few years in both hospitals. We have encountered a variety of problems that I would characterize as “slippery slope” that we continue to struggle with. Let me see if I can describe them:
1. ED physicians and surgeons who are used to getting plasma upfront in the setting of trauma request the MT coolers in other settings: ruptured aortic aneurysm and GI bleeds for example. They have lobbied to get plasma in the first coolers sent for all massive hemorrhage scenarios and the BB does not have the resources to check at the time of request whether the request is appropriate.
I am not overwhelmed by the evidence supporting early plasma transfusion in trauma but am willing to support this practice. I have been unable to convince other providers that they likely do not need plasma immediately in other settings. They argue that patients in these other clinical settings may be coagulopathic as well, and that having plasma and platelets up front let’s them address these coagulopahies.
2. My excellent blood bank techs are getting confused. We had one case, I think this was a GI bleed, where we had a current blood type on the patient, who typed as group B. The techs prepared the cooler with one tech putting in group B red cells and the second the thawed group A plasma. I am concerned the practice of giving group A plasma to all groups in emergency situations relaxes the vigilance we have about giving incompatible plasma.
3. We also have an emergent reversal of coumadin protocol. This is for patients who require very rapid reversal but do not meet criteria for 4 factor concentrate. Do we give these patients A plasma even if have a history that they are group B or group AB? Since we now also have thawed group B plasma, do we give group B plasma based on a historical blood type alone (which we would never do here-to-fore) or do we give group A until we can confirm the blood type on a current specimen? Or do we ask the techs to have a very complicated conversation with clinicians providing emergency care?
This is turning into a huge can of worms with me trying to convince the providers that Group A plasma is safe, but not that safe.
Any thoughts or advice?
Lots to talk about there. I’ll keep to two specific points:
Thanks for writing! I wish you the best. These are challenging situations, and everyone is struggling with the issues you raised, especially in your point 1.
-Joe
Dear Ann,
Thanks for submitting this comment. This is also something we struggle with at my hospital.
For this first scenario, we have addressed this with creation of a separate MTP for trauma patients which can only be activated by Trauma surgeons. This is the only situation in which we use thawed group A plasma for patients of unknown blood type.
Outside of the trauma setting, I would only use the thawed group A plasma if the patient ABO/Rh was known and was compatible with group A plasma (i.e. group O or A). Otherwsie we thaw type specific.
Ongoing education about the rationale for using group A plasma in trauma and the lack of evidence for early plasma provision in other settings is key.
Hope that helps!
Nancy
The faith in the efficacy and safety of early plasma and platelet transfusions (and early red cell transfusions too) is not, in my view, evidence based in the case of non-trauma patients. Even in the trauma setting, and defining coagulopathy as any elevated INR, aPTT, etc., it is not clear that transfusing plasma and platelets in the first shipment or two is beneficial. In any case, this is probably <25% of patients. Thus, to my way of thinking we are giving inappropriate, unnecessary therapy to 75% of patients in hopes of saving some of the other 25%.
Given the known but largely underappreciated toxicity of transfusions (nosocomial infection, thrombosis, and multi-organ failure, in addition to those long accepted), we reserve plasma, cryo and platelet containing "automated" MTP protocols for patients who have received 8 red cells (adults) or who the trauma/ED physicians believe are clinically coagulopathic or have laboratory/TEG evidence for same. We thus avoid unnecessarily treating and harming the preponderance of patients who are not coagulopathic at presentation, and may never become coagulopathic.
I would suggest that ED physicians who want to treat early with platelets and plasma are almost certainly doing more harm than good, and the same goes for red cells, based upon the Barcelona randomized trial of upper GI bleeding in NEJM.
Traditional thinking about the benefits of transfusion need to be rethought, despite the fact that this thinking is time honored. Such assumptions of widespread benefit of transfusion are now known to be in large part wrong.
The randomized trials of restrictive red cell transfusions demonstrate this for RBC. The disappointing and opposite of expected results from platelet and plasma transfusions in randomized trials of reversing anti-platelet drugs and vitamin K antagonists demonstrate this for these two components. Patients who receive treatment with platelets to reverse aspirin/clopidogrel, etc. or who receive plasma to reverse coumadin do significantlyl worse than those patientsreceiving no transfusions, or factor concentrates, respectively. It's contrary to standards of practice, but when the data do not support the standards of practice, it's the data we should honor.
Thank you Dr. Neil Blumberg for your comments. Would you be so kind as to share the name of the study/paper you reference regarding poorer outcomes in reversing anti-platelet drugs and coumadin with components?
Sorry for the late reply:
Bad outcomes with platelet transfusion to reverse anti-platelet drugs in intra-cranial bleeding: Lancet. 2016 Jun 25;387(10038):2605-13. doi: 10.1016/S0140-6736(16)30392-0. Epub 2016 May 10.
Higher mortality with plasma vs. factor concentrate to reverse vitamin K antagonists:
Thromb Haemost. 2016 Oct 28;116(5):879-890. Epub 2016 Aug 4.
What about group A plasma to a group B, or AB recipient if the donor plasma is high antibody titre negative?
I’m not sure what you are asking, Will. This is kind of the point of the discussion above.
-Joe