Transfusing patients with sickle cell disease (SCD) is a big deal, for many reasons. Eric Gehrie guides us through those challenges, especially alloimmunization (making antibodies against red cell antigens).

Dr. Eric Gehrie
Where do RBCs fit in?
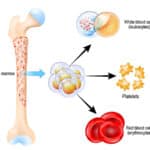
Red blood cell transfusion is a mainstay of therapy in patients with SCD. While lifesaving, especially in regard to stroke prevention and treatment, giving red cells to a patient with SCD is often not as simple as just pulling units off the shelf and transfusing! In this episode, Dr. Gehrie describes some of the things that blood bankers should be thinking when we transfuse RBCs to sickle cell patients. In particular, he helps us work through issues surrounding alloimmunization, which is a massive problem for those with SCD.
(History lesson credit: Bunn HF. Chapter 9: Sickle Cell Disease. Pathophysiology of Blood Disorders, 2nd ed.)

Dr. Eric Gehrie
Where do RBCs fit in?
Red blood cell transfusion is a mainstay of therapy in patients with SCD. While lifesaving, especially in regard to stroke prevention and treatment, giving red cells to a patient with SCD is often not as simple as just pulling units off the shelf and transfusing! In this episode, Dr. Gehrie describes some of the things that blood bankers should be thinking when we transfuse RBCs to sickle cell patients. In particular, he helps us work through issues surrounding alloimmunization, which is a massive problem for those with SCD.
(History lesson credit: Bunn HF. Chapter 9: Sickle Cell Disease. Pathophysiology of Blood Disorders, 2nd ed.)
About My Guest:
Dr. Eric Gehrie is a physician from whom you will be hearing great things in the future! He is currently the Associate Director of Transfusion Medicine and Assistant Professor of Pathology at Johns Hopkins in Baltimore, MD. He did his transfusion medicine fellowship at Yale-New Haven Hospital and was previously the Assistant Director of the Blood Bank and of Apheresis at that hospital. Dr. Gehrie’s clinical and research interests are focused on the safety and efficacy of blood transfusion and therapeutic apheresis. In particular, he is interested in developing algorithms to predict adverse events related to blood transfusion. He is a co-investigator of the National Heart Lung and Blood Institute (NHLBI) supported Recipient Epidemiology and Donor Evaluation Study-III (REDS-III), where he focuses on the impact of blood transfusion on recipient vital signs and pulmonary injury. He also is a co-investigator of a post-marketing surveillance study evaluating the relationship between platelet transfusion and pulmonary injury in hematology/oncology patients. In addition to these efforts, Dr. Gehrie is committed to patient blood management, with a particular emphasis on the development and implementation of evidence-based guidelines for the initiation of blood component transfusion. Shortly after this podcast was recorded, Dr. Gehrie was named as one of the ASCP’s “40 under 40” honorees as recognition of his leadership and achievements.
Further Reading:
- Responder/Non-responder Discussion (NOTE: Be patient; the article may take a few minutes to come up): Gehrie EA and Tormey CA. The Influence of Clinical and Biological Factors on Transfusion-Associated Non-ABO Antigen Alloimmunization: Responders, Hyper-Responders, and Non-Responders. Transfus Med Hemother 2014;41:420-429 (free access at time of episode release)
- Sickle Cell Alloimmunization Despite Matching: Chou ST et al. High prevalence of red blood cell alloimmunization in sickle cell disease despite transfusion from Rh-matched minority donors. Blood 2013;122:1062-1071.









Thank you Dr. Chaffin!
This great podcast made my learning more interesting and easy to understand.
Excellent teacher